Quality of Life in Patients with Central Post-Stroke Pain in Riau, Indonesia: A Cross-Sectional Study
Main Article Content
Abstract
Background: Central Post-Stroke Pain (CPSP) is a chronic neuropathic complication of stroke that substantially impairs long-term well-being. While its clinical characteristics are increasingly recognized, data regarding the multidimensional quality of life (QoL) impact of CPSP in regional Indonesian populations remain limited. This study aimed to describe the QoL profile of CPSP patients at Arifin Achmad General Hospital to provide a comprehensive understanding of the disease burden.
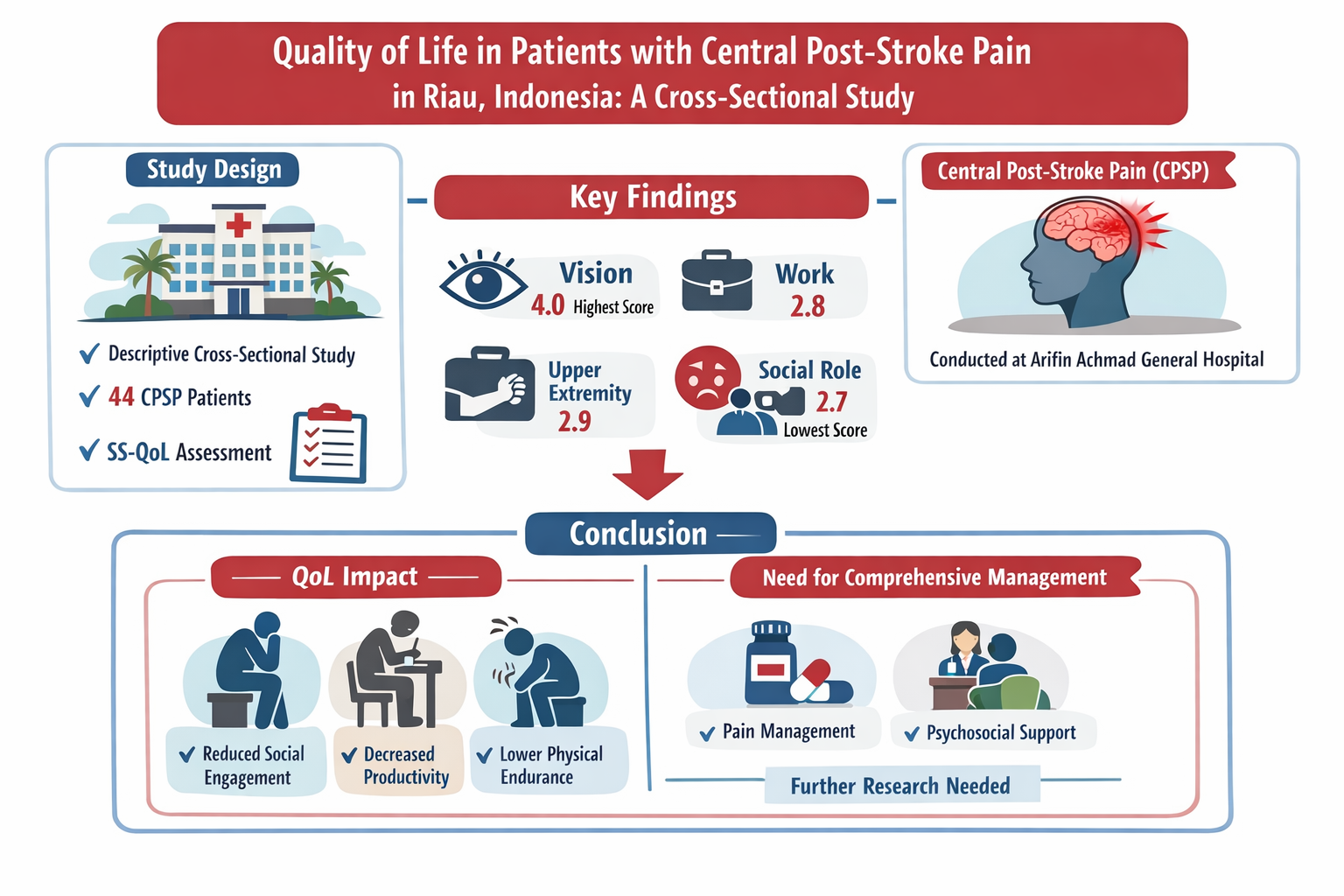
Methods: A descriptive cross-sectional study was conducted from August to October 2025 at the Neurology Outpatient Clinic of Arifin Achmad General Hospital, Riau. Forty-four patients diagnosed with CPSP were included. QoL was assessed using the validated Indonesian version of the Stroke-Specific Quality of Life (SS-QoL) scale. Descriptive univariate analysis was performed to determine median scores across domains.
Results: QoL scores demonstrated marked heterogeneity across domains. The Vision domain showed the highest median score (4.0), whereas Social Role recorded the lowest (2.7). Notable reductions were observed in Work, Upper Extremity Function, and Energy domains. In contrast, Language and Self-care domains were relatively preserved. These findings indicate that although basic functional abilities may remain intact, CPSP significantly compromises social participation, occupational capacity, and physical activity.
Conclusion: CPSP imposes a substantial multidimensional burden, particularly affecting social engagement, productivity, and physical endurance. Comprehensive management strategies extending beyond pharmacological pain control are essential to address the psychosocial and functional consequences of CPSP. Further longitudinal studies with larger sample sizes are needed to clarify determinants of QoL outcomes in this population.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
How to Cite
References
Feigin VL, Abate MD, Abate YH, ElHafeez SA, Abd-Allah F, Abdelalim A, et al. Global, regional, and national burden of stroke and its risk factors, 1990–2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet Neurol. 2024;23(10):973-1003.
Widyadharma IPE, Tertia C, Wijayanti IAS, Barus JFA. Central post-stroke pain: what are the new insights? Rom J Neurol. 2021;20(1):28-34.
Betancur DFA, Tarragó MGL, Torres ILS, Fregni F, Caumo W. Central post-stroke pain: an integrative review of somatotopic damage, clinical symptoms, and neurophysiological measures. Front Neurol. 2021;12:717106.
Hartley T, Burger M, Inglis-Jassiem G. Post-stroke health-related quality of life, stroke severity and function: a longitudinal cohort study. Top Stroke Rehabil. 2020;27(1):1-10.
Sekeon SAS, Adisasmita A, Sudaryo MK, Tantri AR. Prevalence and impact of central post-stroke pain on quality of life among stroke survivors: a cross-sectional study. Acta Med Indones. 2025;57(1):52-60.
Yuan X, Hu S, Fan X, Jiang C, Xu Y, Hao R, et al. Central post-stroke pain: advances in clinical and preclinical research. Stroke Vasc Neurol. 2024;9:1-16.
Gandolfi M, Donisi V, Battista S, Picelli A, Val N, Del Piccolo L, et al. Health-related quality of life and psychological features in post-stroke patients with chronic pain: a cross-sectional study in the neuro-rehabilitation context of care. Eur J Phys Rehabil Med. 2021;57(4):620-629.
Li CC, Tsai SJ, Tai JC, Wu TJ, Tsai SM, Kao SC, et al. Association between family functioning and health-related quality of life in stroke survivor–informal family caregiver dyads. Asian Nurs Res (Korean Soc Nurs Sci). 2024;18(2):141-147.
Ösken S, İçağasıoğlu A, Durmuş B, Sağ S, Madenci E. Frequency of central post-stroke pain and its impact on quality of life. Sak Med J. 2022;12(2):89-96.
Tang SC, Lee LJH, Jeng JS, Hsieh ST, Chiang MC, Yeh SJ, et al. Pathophysiology of central poststroke pain: motor cortex disinhibition and its clinical and sensory correlates. Stroke. 2019;50(10):2851-2857.
Mohanan AT, Nithya S, Nomier Y, Hassan DA, Jali AM, Qadri M, et al. Stroke-induced central pain: overview of the mechanisms, management, and emerging targets of central post-stroke pain. Pharmaceuticals (Basel). 2023;16(8):1098.
Payton H, Soundy A. The experience of post-stroke pain and the impact on quality of life: an integrative review. Disabil Rehabil. 2020;42(14):1981-1991.
Kam JE, Choo PL. Feeling lonely and dissatisfied: understanding social network functioning in stroke survivors. Int J Environ Res Public Health. 2024;21(3):1234.
Anosike KC, Rajaram Manoharan SVR. Central post-stroke pain syndrome. StatPearls Publishing; 2024. [Last accessed on 2024 Oct 31]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK604196/
Barbosa LM, Silva VA, Rodrigues ALL, Fernandes DTRM, Oliveira RDSAA, Galhardoni R, et al. Dissecting central post-stroke pain: a controlled symptom-psychophysical characterization. Brain Commun. 2022;4(3):fcac142.
Saar KTAPAT. Returning to work after stroke: associations with cognitive function. J Stroke Cerebrovasc Dis. 2023;32(5):106987.
Chen J, Wang X, Xu Z. The relationship between chronic pain and cognitive impairment in the elderly: a review of current evidence. J Pain Res. 2023;16:2309-2319
Yuan X, Hu S, Fan X, Jiang C, Xu Y, Hao R, et al. Central post-stroke pain: advances in clinical and preclinical research. Stroke Vasc Neurol. 2024;9:1-16.
Suñer-Soler R, Maldonado E, Rodrigo-Gil J, Font-Mayolas S, Gras ME, Terceño M, et al. Sex-related differences in post-stroke anxiety, depression and quality of life in a cohort of smokers. Brain Sci. 2024;14(2):210.
Sütçü Uçmak G, Kılınç M. The effects of kinesiophobia, fatigue, and quality of life on physical activity in patients with stroke. Top Stroke Rehabil. 2024;31(8):788-794.