Maternal Factors and Their Relationship with Low Birth Weight: Evidence from a Case-Control Study
Main Article Content
Abstract
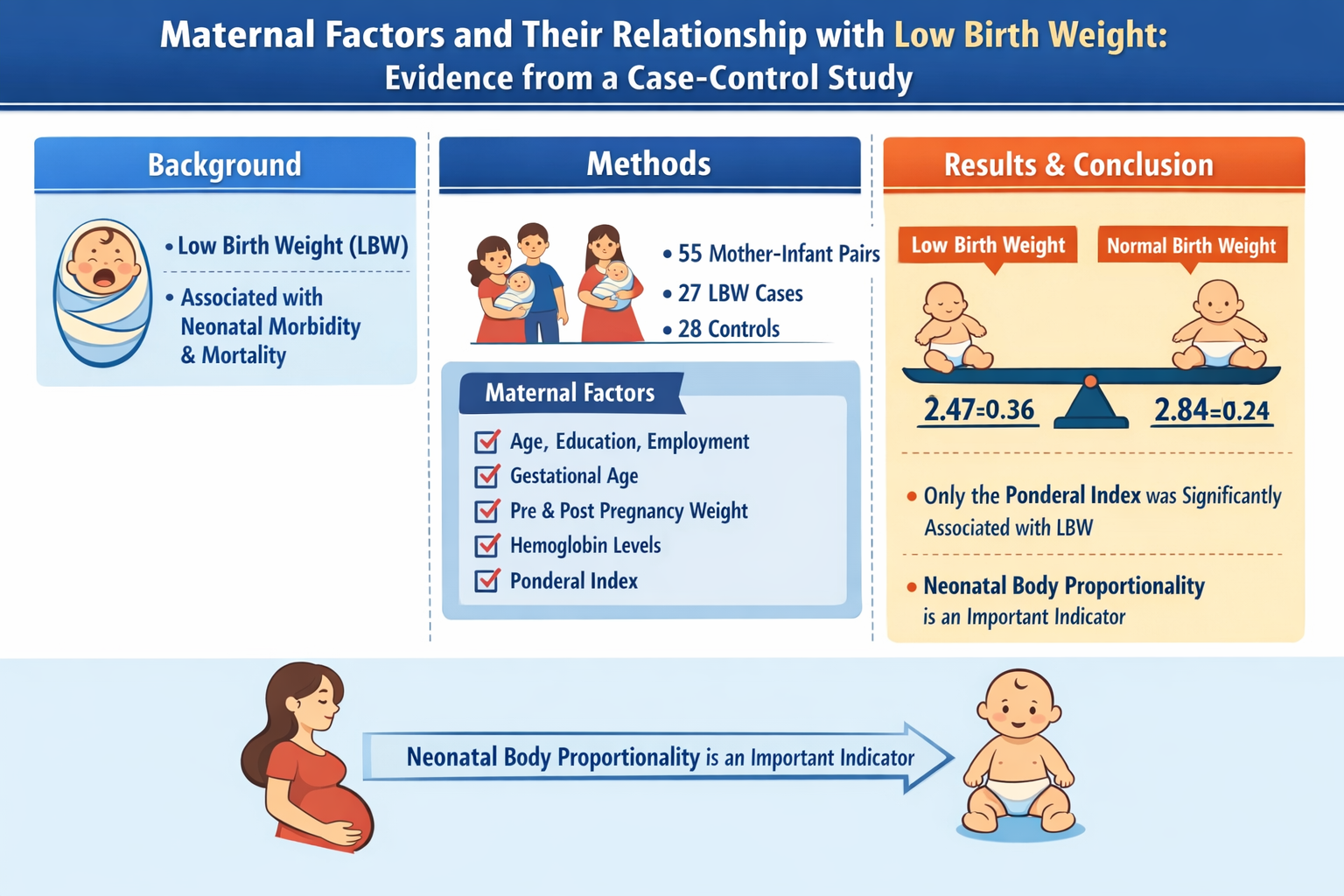
Background: Low birth weight (LBW) remains a major public health concern due to its association with neonatal morbidity and mortality. Maternal factors during pregnancy may influence birth weight outcomes. This study aimed to examine the relationship between maternal factors and low birth weight using a case-control design.
Methods: A case-control study was conducted involving 55 mother–infant pairs, consisting of 27 LBW cases and 28 normal birth weight controls. Maternal characteristics, including age, education, employment status, gestational age, pre-pregnancy weight, post-pregnancy weight, hemoglobin levels before and after pregnancy, and infant sex, were collected. The ponderal index was also assessed. Categorical variables were analyzed using appropriate comparative tests, and continuous variables were compared using mean differences. A p-value <0.05 was considered statistically significant.
Results: Most mothers were aged 20–35 years (80.0%) and unemployed (76.4%). Nearly half had completed senior high school (49.1%). There were no significant associations between infant sex, maternal age, education, employment status, gestational age, pre-pregnancy weight, post-pregnancy weight, hemoglobin levels before pregnancy, or hemoglobin levels after pregnancy and birth weight outcome (p>0.05). However, the mean ponderal index was significantly lower in the LBW group compared to the normal birth weight group (2.47±0.36 vs. 2.84±0.24; p<0.001).
Conclusion: Among the maternal factors examined, only the ponderal index showed a significant association with low birth weight. These findings suggest that neonatal body proportionality may be an important indicator related to birth weight outcomes.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
How to Cite
References
Mahmudiono T, Nindya TS, Andrias DR, Megatsari H, Rosenkranz RR. Household food insecurity as a predictor of stunted children and overweight/obese mothers (SCOWT) in urban Indonesia. Nutrients. 2018; 10:535
Masrul M, Nindrea RD, Sudji IR, Purnakarya I. Cut off point of insulin-like growth factor-1 (IGF-1) for prediction of child stunting. Indian J Public Health Res Dev. 2020; 11(1): 1234-9.
Hendriyani H, Sudargo T, Lusmilasari L, Helmyati S, Susetyowati S, Nindrea RD. Complementary Feeding Self-efficacy: A Concept Analysis. Open Access Maced J Med Sci. 2020; 8(F):11-2.
Masrul M, Izwardy D, Sudji IR, Purnakarya I, Syahrial S, Nindrea RD. Microbiota Profile with Stunting Children in West Sumatera Province, Indonesia. Open Access Maced J Med Sci. 2020;8(E):334-40.
Nindrea RD, Rosalina L, Novera M, Ming LC, Sari NP, Avilla NA, Putri FAR, Rivani NP. Assessing maternal postnatal depression, bonding and practices in mothers of preterm and low birth weight infants in Indonesia. MethodsX. 2025 Dec 5;16:103750.
Alristina AD, Laili RD, Nagy É, Feith HJ. The Importance of Socioeconomic Factors Associated with Maternal Nutrition Knowledge and Undernutrition Among Children Under Five. Nutrients. 2025;17(21):3355.
Aji RS, Efendi F, Kurnia ID, Tonapa SI, Chan CM. Determinants of maternal healthcare service utilisation among Indonesian mothers: A population-based study. F1000Res. 2021;10:1124.
Mahamud Tohan M, Islam MA, Rahman MA. Exploring the factors behind socioeconomic inequalities in Antenatal Care (ANC) utilization across five South Asian natiaons: A decomposition approach. PLoS One. 2024;19(8):e0304648.
Has EMM, Efendi F, Wahyuni SD, Lailiah N, Mahendra RAP. Predictors of Survival in Under-Five Children with Low Birth Weight: A Population-Based Study in Indonesia. Nurs Rep. 2025;15(7):238.
Sulistiawan D, Bai CH. Pathway linking unwanted pregnancy to low birth weight in Indonesia: A conditional mediation analysis. Heliyon. 2024;10(18):e37565.
Geberu DM, Baffa LD, Hagos A, Tiruneh MG, Teshale G, Tafere TZ, et al. Pooled prevalence and factors of low birth weight among newborns in the top 20 countries with the highest infant mortality: analysis of recent demographic and health surveys. BMJ Open. 2025;15(4):e098090.
Wulandari F, Mahmudiono T, Rifqi MA, Helmyati S, Dewi M, Yuniar CT. Maternal Characteristics and Socio-Economic Factors as Determinants of Low Birth Weight in Indonesia: Analysis of 2017 Indonesian Demographic and Health Survey (IDHS). Int J Environ Res Public Health. 2022;19(21):13892.
Čvorović J. The Association Between Maternal Age at Childbirth and Child Nutritional Outcomes: A Cross-sectional Study From Serbian Roma Communities. Glob Pediatr Health. 2024;11:2333794X241298831.
Abebe YM, Deribe L, Fantahun A, Beyene BN, Megule SM, Shiferaw WG, et al. Advanced maternal age increases the risk of adverse neonatal outcomes: a comparative study in Ethiopia. BMC Pregnancy Childbirth. 2025;25(1):1144.
Lackovic M, Jankovic M, Mihajlovic S, Milovanovic Z, Rovcanin M, Mitic N, Nikolic D. Gestational Weight Gain, Pregnancy Related Complications and the Short-Term Risks for the Offspring. J Clin Med. 2024;13(2):445.
Hochstedler KA, Bell G, Park H, Ghassabian A, Bell EM, Sundaram R, et al. Gestational Age at Birth and Risk of Developmental Delay: The Upstate KIDS Study. Am J Perinatol. 2021;38(10):1088-1095.
Nawsherwan, Khan A, Begum N, Ahmed Z, Mubarik S, Haq IU, Nabi G, Ullah N, Fan C, Wang S. Low Birth Weight, and Low Ponderal Index Mediates the Association between Preeclampsia, Placenta Previa, and Neonatal Mortality. Iran J Public Health. 2020;49(4):654-662.
Hwang JK, Kang HN, Ahn JH, Lee HJ, Park HK, Kim CR. Effects of Ponderal Index on Neonatal Mortality and Morbidities in Extremely Premature Infants. J Korean Med Sci. 2022;37(24):e198.
Wium-Andersen MK, Jørgensen TSH, Jørgensen MB, Rungby J, Hjorthøj C, Sørensen HJ, Osler M. The association between birth weight, ponderal index, psychotropic medication, and type 2 diabetes in individuals with severe mental illness. J Diabetes Complications. 2022;36(5):108181.
Liu Q, Wen J, Fang L, Huang Y, Rao T, Shi X, Wu J. Birth weight and ponderal index percentiles for twins based on sex and chorionicity in a center of Guangdong Province, China. Transl Pediatr. 2024;13(12):2221-2232.